Claims shouldn’t be a guessing game. Sunbound combines AI-driven scrubbing with expert human intervention to prevent denials before submission and overturn rejections faster.
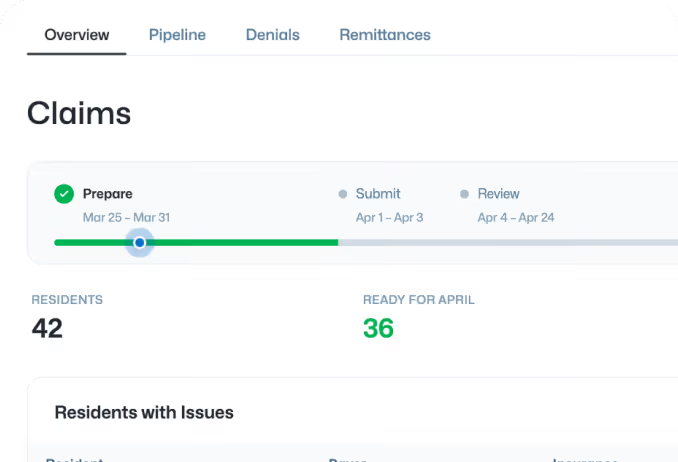
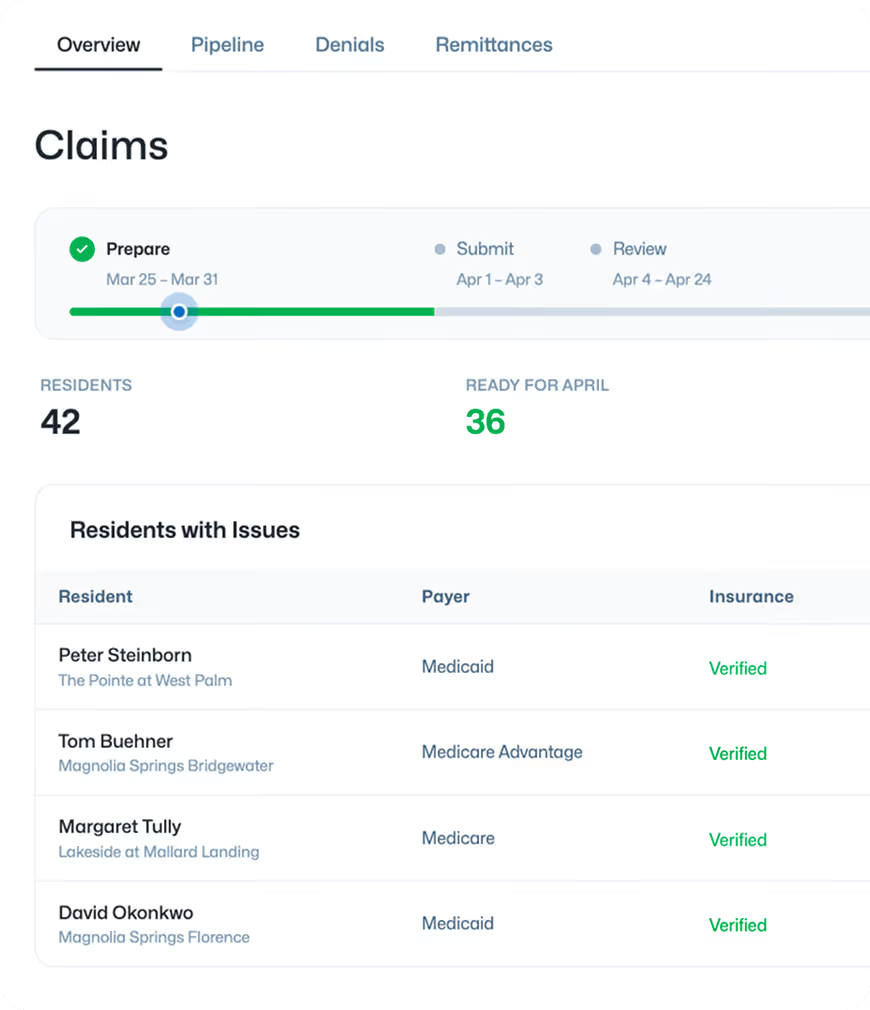






Effective denial management in senior living is not just about appealing rejected claims; it is about preventing them through rigorous front-end eligibility checks and pre-submission scrubbing. While the industry average denial rate hovers around 15-20%, a robust RCM strategy typically lowers this to under 5% by catching coding errors and authorization gaps before they reach the payer.
With Sunbound, operators typically see:
claims acceptance.
in reimbursement revenue.
by catching issues before they surface.

From PDPM shifts in Skilled Nursing to state-specific Medicaid waivers in Assisted Living, keeping up with payer rules is a full-time job. One wrong code triggers a denial that takes weeks or months to catch and fix.

Once a claim is submitted, most teams have no idea where it sits. Is it pending, processing, or rejected? You find out once a paper EOB arrives 45 days later. You proactively can’t fix what you can’t see.

Your BOMs are experts in resident care, not insurance bureaucracy. Forcing them to spend hours on hold with payers leads to burnout, turnover, and neglected resident families. Have them focus on care instead.

Medicaid and Managed Care plans require constant re-authorization. If these dates are missed due to manual tracking, you essentially provide care for free, with zero chance of reimbursement.
Sunbound ensures every claim is eligible, accurate, and complete before it goes out the door, dramatically reducing denials across your portfolio.

Swap manual phone tag for a frictionless digital payment experience. Automated reminders keep resident balances current and help our our partners collect on 99%.

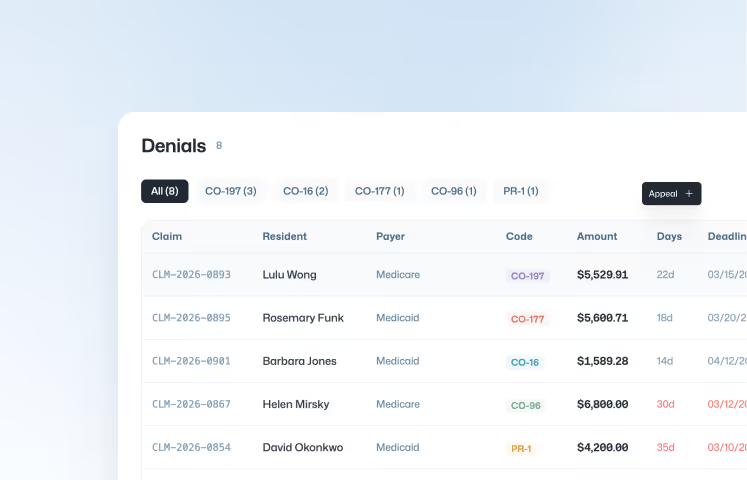
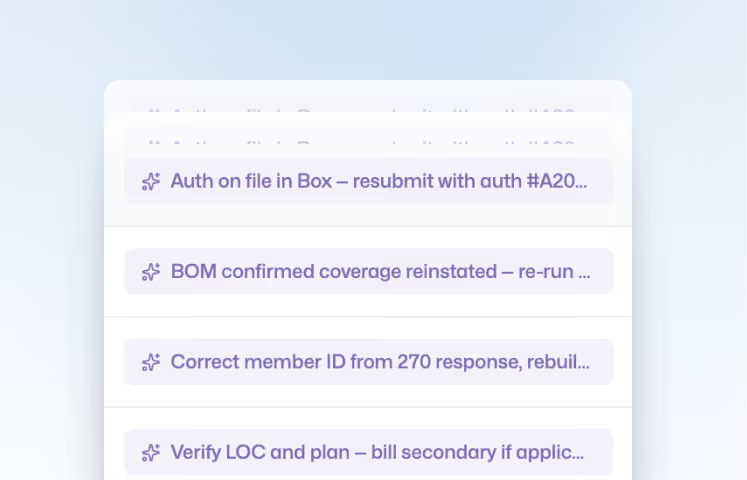
Prevent rejections by checking eligibility and coding errors pre-submission. When denials occur, our experts aggressively appeal them to keep bad debt near $0.

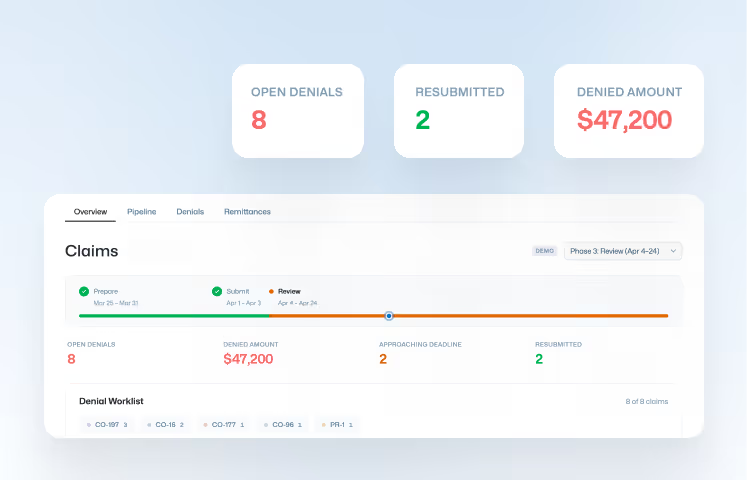
Get real-time visibility into your revenue cycle with a live dashboard. Intervene days after a missed payment rather than waiting for month-end reports to reveal the damage.


"Sunbound has made a real difference in how our teams operate day to day. It’s reduced the administrative load, improved efficiency and allowed our staff to stay focused on our residents. Our ROI has improved through their collection efforts and just as important, the Sunbound team is incredible to work with and truly delivers on what they promise."
Every day an invoice sits unpaid, it becomes harder to collect. Secure your revenue today.




Speed is critical. We typically initiate the appeal process within 48 hours of receiving a denial. By acting immediately, we ensure we are well within the "timely filing" limits and keep the revenue cycle moving.

When a resident is approved for Medicaid months after admission, we automatically identify the "retro period" and generate the necessary claims to capture that back-pay. We track the approval dates and ensure the billing window is utilized fully before it expires.

You have full transparency. Our dashboard integrates directly with the clearinghouse to show you real-time status updates (e.g., "Accepted," "Pending," "Paid"). You never have to log into a separate portal or call a payer to know where your money is.

Absolutely. Managed Care plans often have unique "level of care" codes and aggressive denial tactics. We maintain a database of specific rules for major payers (United, Humana, Aetna) to ensure your claims meet their arbitrary formatting requirements every time.

Yes. While your clinical team determines the assessment, Sunbound ensures that the HIPPS codes on the claim match the MDS assessment data exactly. We scrub for consistency to prevent audits and recoupments related to PDPM mismatch errors.