Stop Leaving MCO Money on the Table
End-to-end Medicaid and MCO claims management with a nationally trusted, intelligent solution. Streamline everything from eligibility verification to authorizations, and denial management. Operators see a reduction in bad debt, faster reimbursement, and less staff burden.


Trusted by Leading Operators and Partners






Predictable Claims Reimbursement
Clarity, control, and peace of mind for Medicare and Medicaid claims.
Claims Shouldn’t Feel Like a Mystery
Managing Medicare and Medicaid claims is complex, compliance-driven, and time-sensitive.
When processes are fragmented or opaque, reimbursements slow, denials rise, and aging balances put pressure on cash flow and planning.
Bad Debt is Preventable
Don't create risks before billing even begins with bad upfront claims.
When eligibility issues aren’t identified early, denials increase, balances age, and revenue that should be reimbursed gets written off as bad debt.
Lack of Visibility Creates Risk
Disconnected systems make it difficult to understand where claims stand at any given moment.
Not knowing what’s submitted, pending, or denied delays action, increases aging, and leaves operators reactionary instead of proactive.
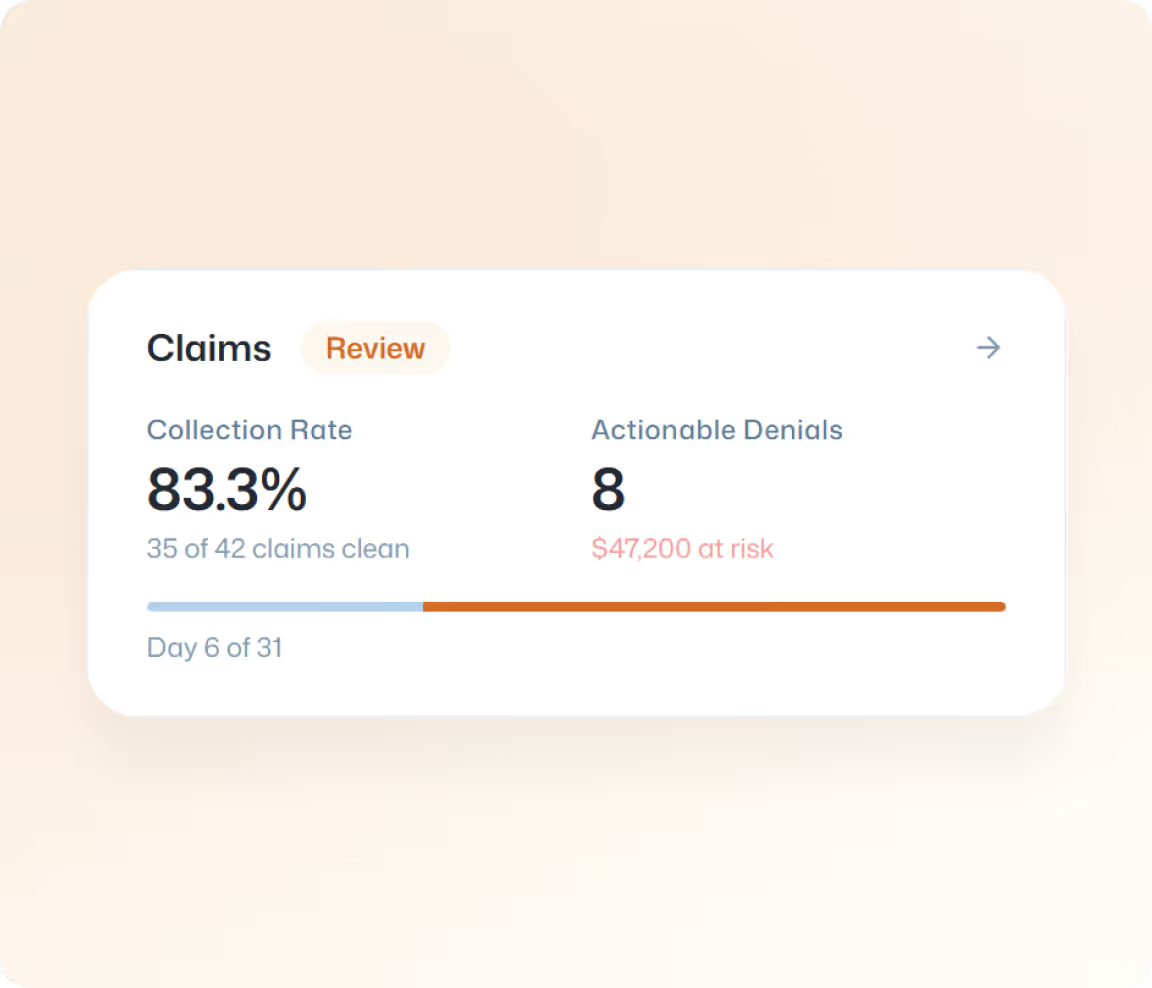
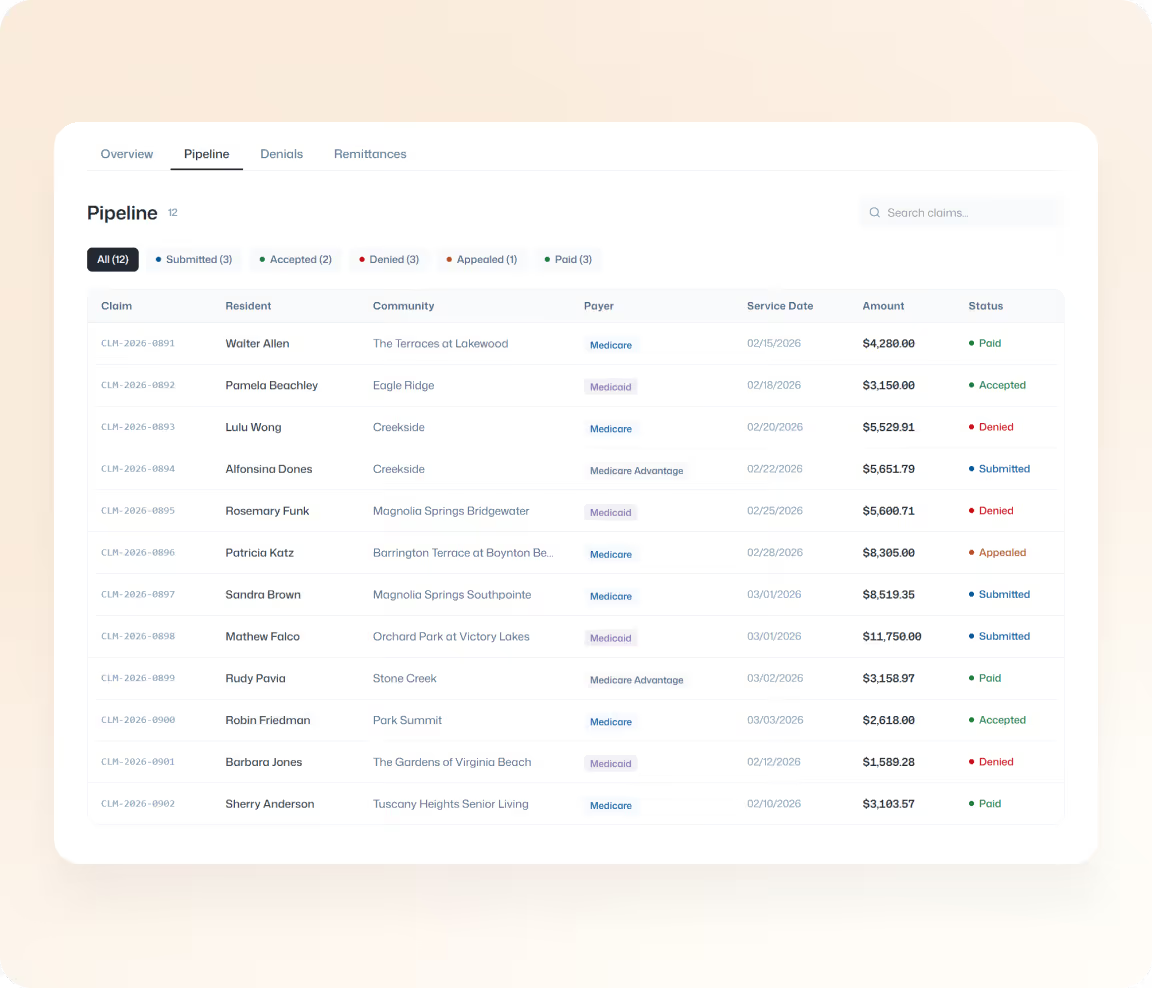
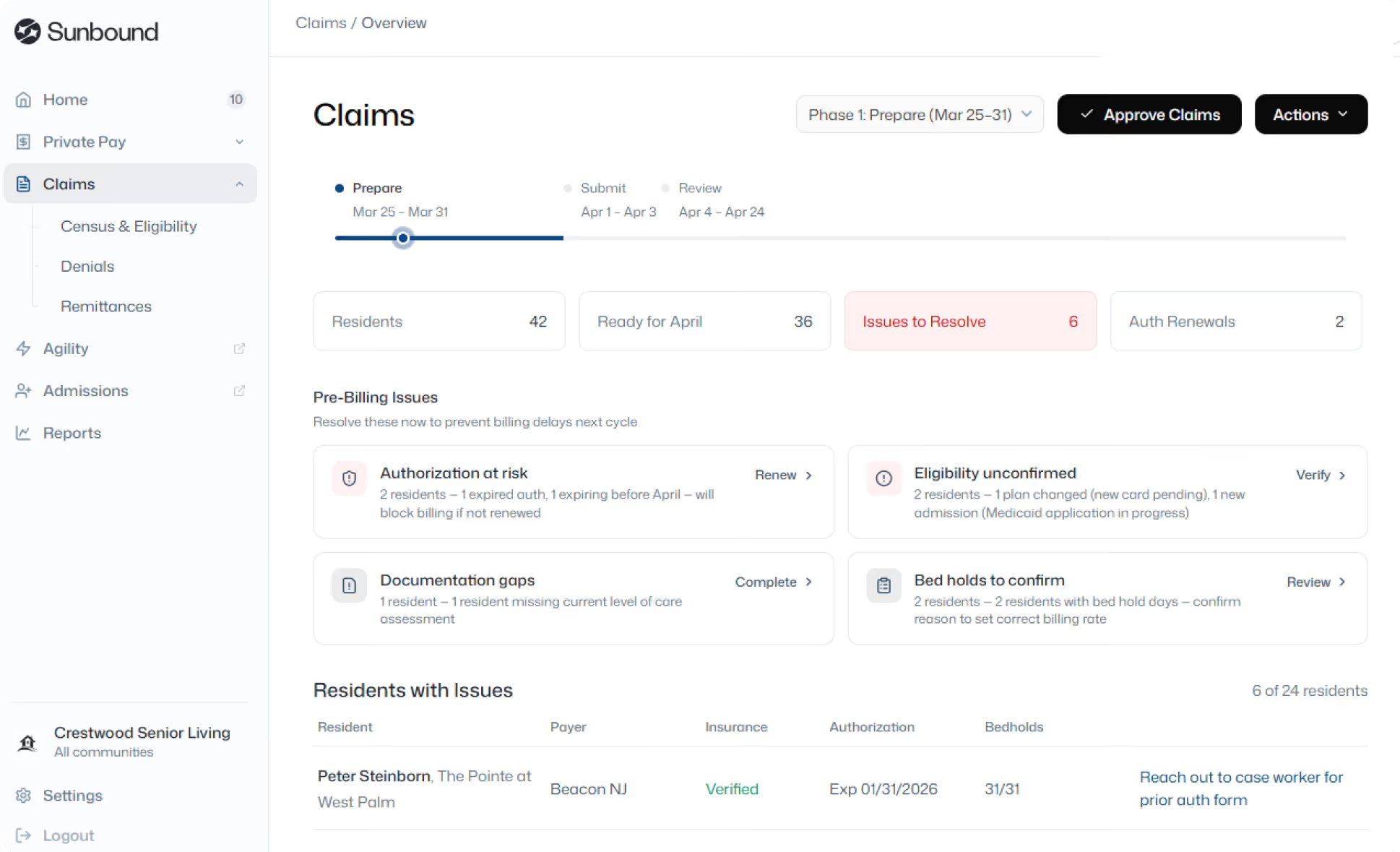
Claims Shouldn’t Feel Like a Mystery
Managing Medicare and Medicaid claims is complex, compliance-driven, and time-sensitive.
When processes are fragmented or opaque, reimbursements slow, denials rise, and aging balances put pressure on cash flow and planning.
Modern Claims, Built to Run Reliably
Claims workflows are organized around the reimbursement lifecycle, with clear phases, checks, and next steps at every stage.

Eligibility Verification
Prevent issues before submission.


Smart Workflows
Smart workflows replace guesswork.


Denial Management
Denials don’t linger.


Real-Time Visibility
No more claims black box.

National Coverage
Built to scale nationwide.

Eligibility Verification
Eligibility is verified upfront to identify coverage gaps, authorization issues, and payer requirements early, reducing denials, preventing aging, and protecting revenue before claims are submitted.
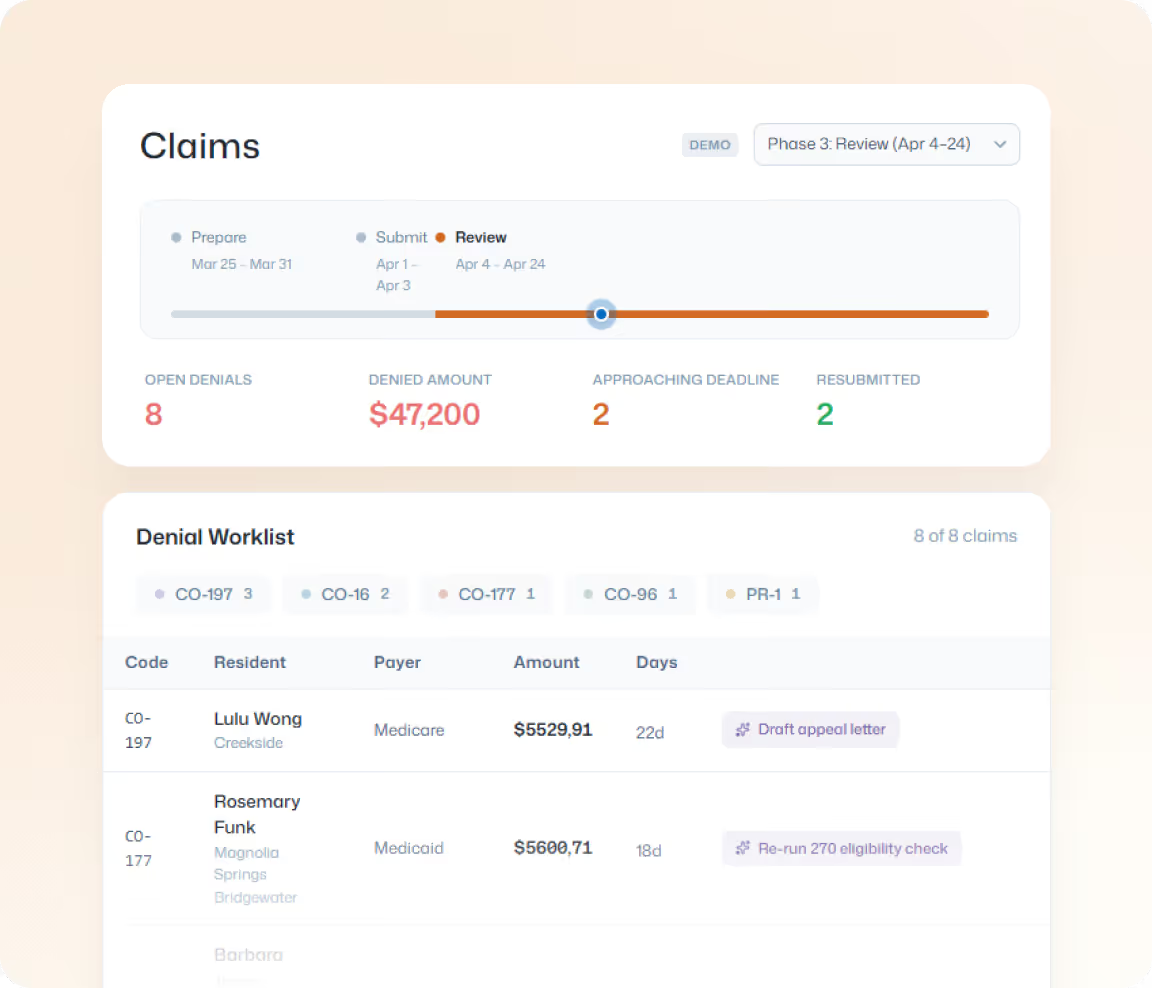

Smart Workflows
Claims move through system-guided stages aligned to the reimbursement lifecycle, with clear checkpoints, ownership, and next steps that keep work organized and on track.
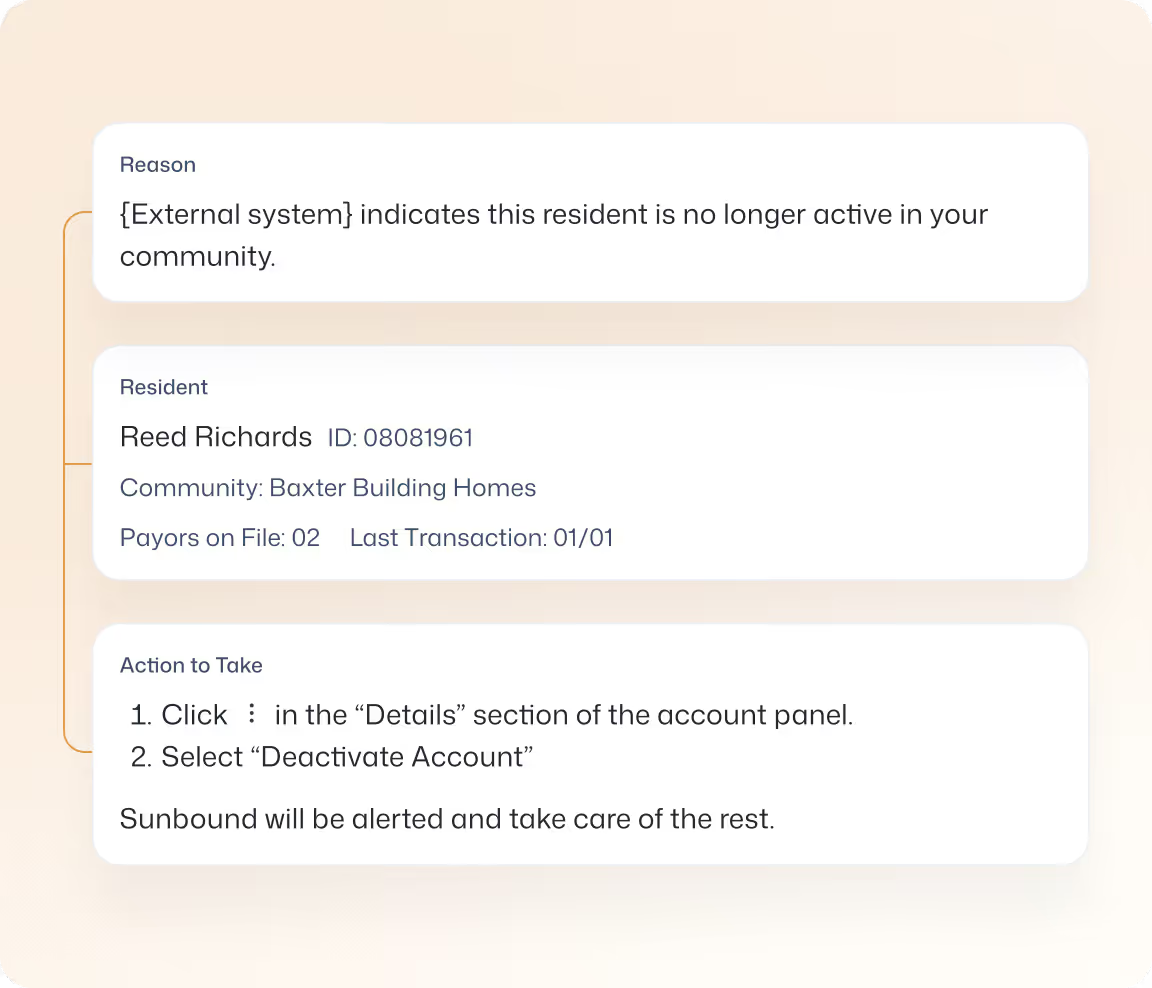

Denial Management
Potential issues are surfaced early and denials are actively tracked through to resolution, helping teams act faster, reduce rework, and shorten reimbursement timelines.
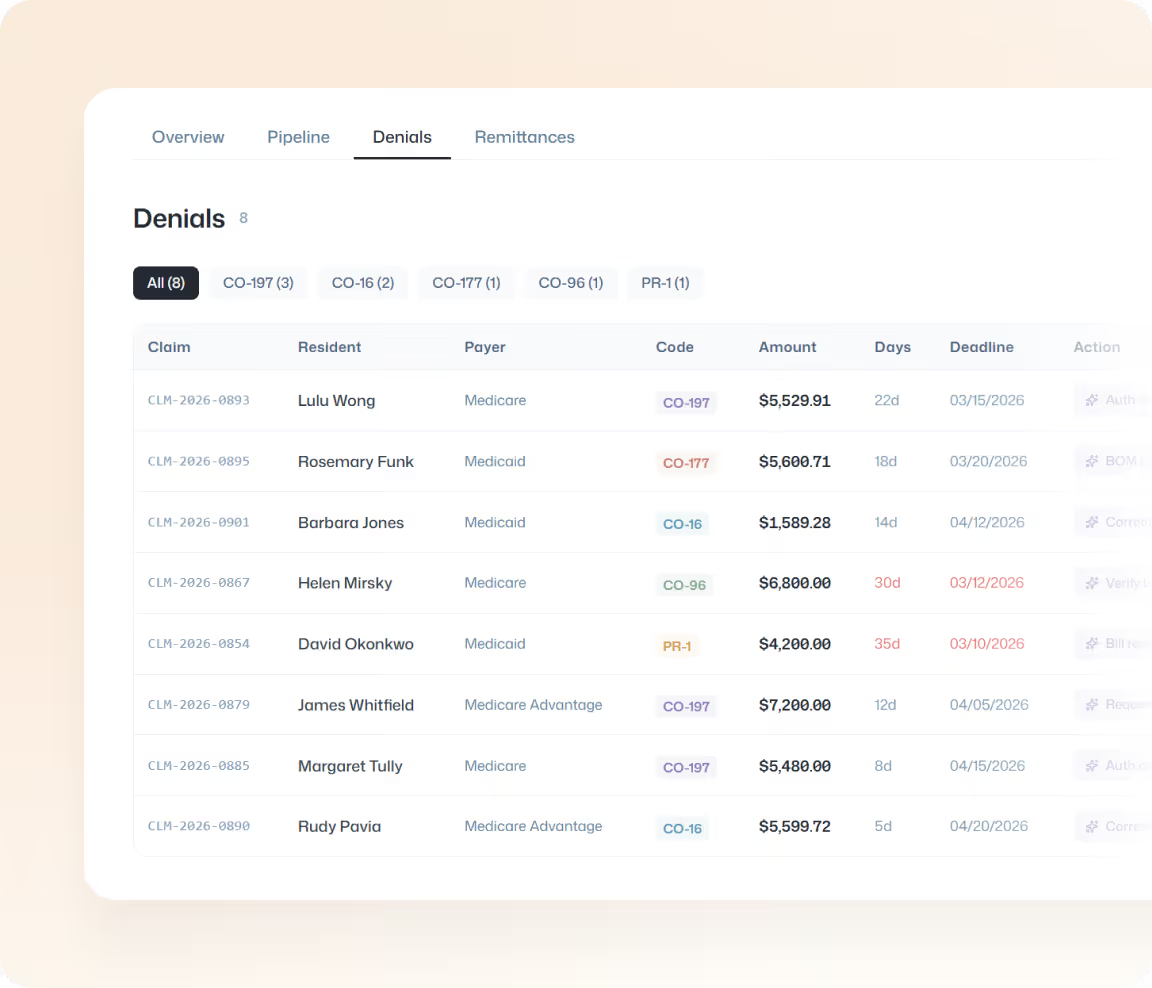

Real-Time Visibility
Real-time visibility shows what’s submitted, pending, denied, or paid across every community, enabling faster intervention, clearer reporting, and fewer surprises.

Systems Integrations
Claims are managed consistently across Medicare and Medicaid programs nationwide, with built-in payer knowledge to support compliant, scalable reimbursement.


Expert Claims Management Without the Administrative Burden
Align Your Standards
Map your portfolio-wide goals to a consistent, best-practice claims playbook to ensure operational predictability.
Verify Eligibility
We help gather resident information early to confirm eligibility and prevent future denials before they happen.
Manage Submissions
Our expert team manages the full billing and resubmission cycle to ensure every dollar of care is collected.
Reconcile with Your EHR
Reimbursements are matched to invoices for real-time reconciliation, audit compliance, and a faster month-end close.
Intelligent Claims Management
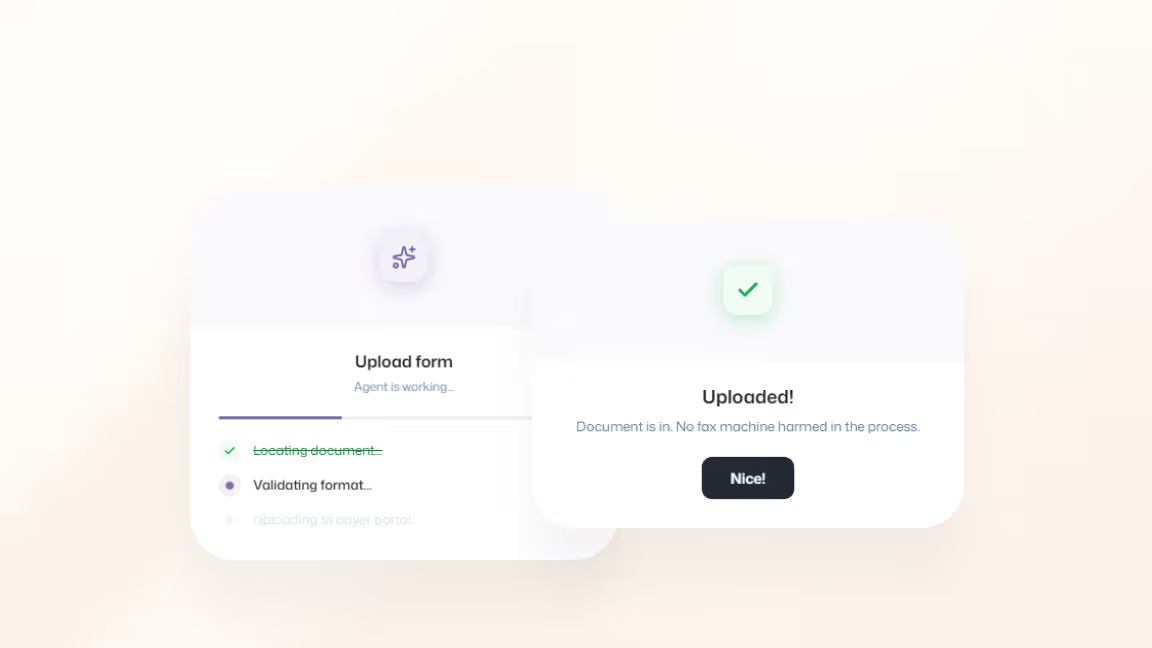
Eligibility errors create downstream risk
Eligibility, coverage, and intake checks happen upfront to catch gaps before submission. As a result, denials decrease, aging is reduced, and reimbursement is protected.
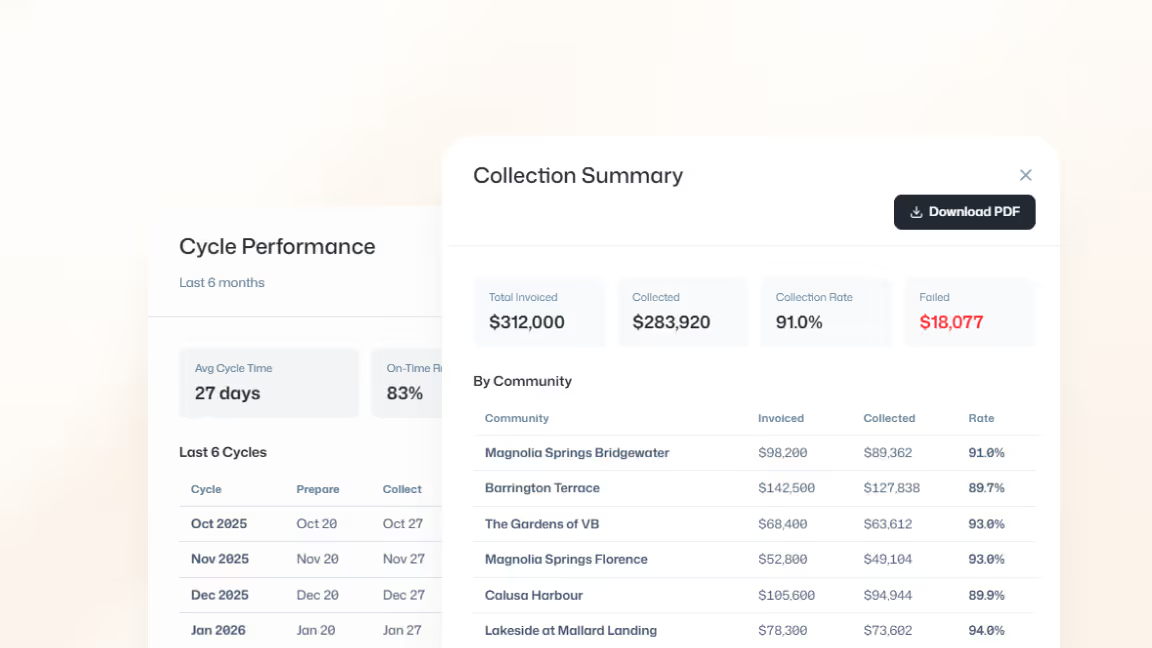
Without visibility, action stalls
See what’s submitted, pending, denied, or paid across every community. Leaders finally have confidence in forecasting and reporting, with clear next steps.
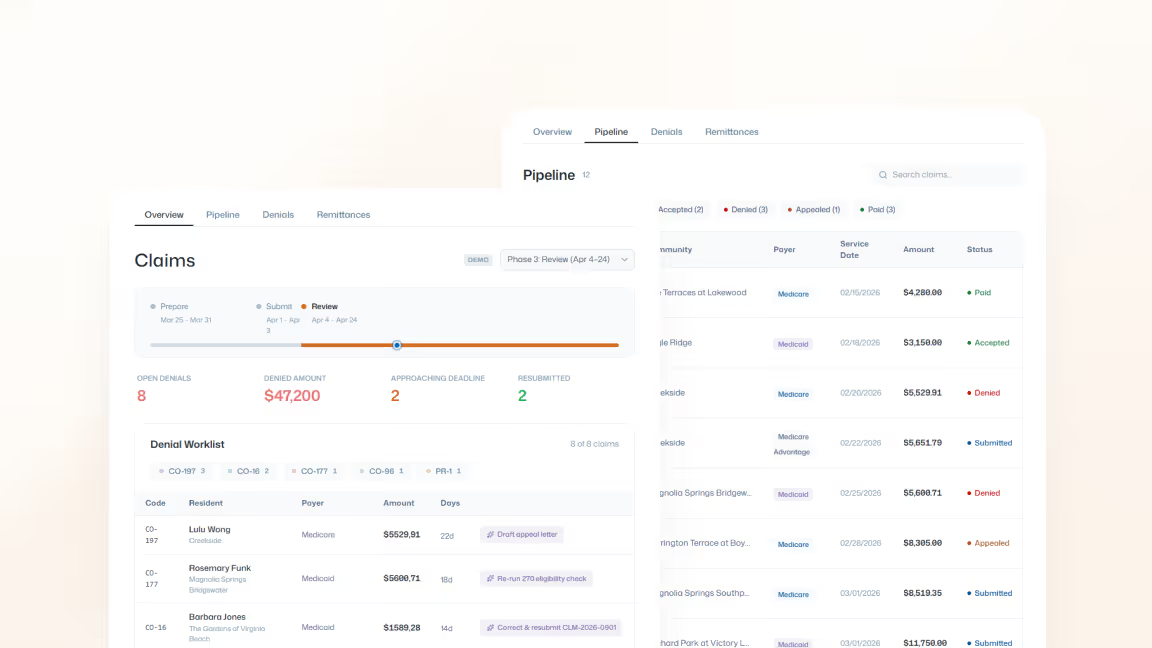
Follow-up shouldn’t be reactive
Denials are actively tracked through resolution so issues don’t stall. Guided follow-up keeps work moving and shortens reimbursement timelines without manual chasing.
The small details matter
Claims are reviewed within structured workflows that bring together clinical and payer requirements. Discrepancies are resolved early, before they impact your close.
Confidence in Every Claim
Claims shouldn’t require constant checking, chasing, or second-guessing. Work is organized around clear phases, proactive checks, and real-time visibility so teams always know where each claim stands.
That clarity reduces denials, shortens reimbursement cycles, and replaces uncertainty with control. Leaders gain confidence that claims are being handled the right way, with the right oversight, even as scale, complexity, and regulatory demands continue to grow.
First-Pass Acceptance Rate
Claims are accepted correctly the first time.
Aging and Bad Debt
Catch issues before they turn into aging.
Avg. Increase in Reimbursement Revenue
Fewer denials mean more revenue realized.
Net Collection Rate
Reimbursement arrives as expected.
Predictable Cash Flow at Scale
Maplewood Senior Living had built an impressive portfolio of 17 communities across six states, but their payment operations hadn't kept pace with their growth.
Partnering with Sunbound, Maplewood streamlined how payments were collected, processed, and reconciled, allowing them to reclaim five full business days each month, and creating predictable, reliable cash flow across all communities.





Protect Your Bottom Line
You can’t control interest rates or labor markets. But you can control your revenue cycle.

Admissions
AI Risk Screening

Private Payments
Faster Payments
Payments

Claims Management
Collect More
Claims Management FAQs
What's the difference between Sunbound's claims management and a billing service or consultancy?

Sunbound is software, augmented by an expert team. Traditional billing services rely entirely on people performing manual work — limiting visibility, scalability, and consistency. Sunbound's platform handles eligibility verification, claim scrubbing, and denial tracking through automation, with expert claims specialists handling escalations and appeals. The result: lower cost, more visibility, and consistent quality across your portfolio.
How does Sunbound improve first-pass claim acceptance rates?

Sunbound's claim scrubbing checks eligibility, authorization status, coding accuracy, and payer-specific requirements before submission. Catching issues pre-submission means claims are accepted on first pass at 96%+ rates, vs. industry averages closer to 80-85%.
Does Sunbound handle Medicaid claims, Medicare claims, or both?

Both. Sunbound manages the full payer mix common in senior living and skilled nursing — Medicaid (state and MCO), Medicare Part A and Part B, Medicare Advantage, VA, and managed care plans. National coverage means consistent workflows regardless of which states your communities operate in.
How does Sunbound's denial management work?

Denials are surfaced in real time as they come back from payers. The platform routes denials to the right specialist, tracks resolution timelines, and provides templated appeal workflows for common denial reasons. The goal is to resolve denials within days, not weeks — which materially improves cash recovery.
What does the implementation timeline look like?

Implementation typically takes 4-8 weeks, depending on portfolio size and current state. Single-community implementations can go live in under 4 weeks; multi-site portfolios with multiple EHRs typically take 6-8 weeks. Your team experiences minimal disruption — Sunbound runs the heavy lifting.



